About SEDRIC
The Surveillance and Epidemiology of Drug-resistant Infections Consortium (SEDRIC) is a think tank designed to bring together a range of international experts to share expertise and take action to tackle the gaps in drug-resistant infection surveillance and epidemiology.
Our mission and aims
Theory of Change
SEDRIC is a think tank with global representation promoting the power of high quality data to tackle Antimicrobial Resistance, made possible through funding support from Wellcome and thanks to input from experts in epidemiology, surveillance, infectious disease and global health. SEDRIC aims to support improvements in data capture and exchange in order to advise public health practitioners, increase AMR awareness and inform funding strategies for AMR surveillance and epidemiology.
SEDRIC approaches the challenge of AMR through three main strategies:
- Our working groups bring together a wide range of experts who provide technical analysis.
- Through our publications, summary papers and consultancy we generate high quality advice.
- Our global meetings, social media presence and tools for strategy allow SEDRIC to play an important role in AMR advocacy.
SEDRIC produces recommendations to bring about sustainable policy change and practice. Through our social media platforms and engagement activities (working groups, workshops and global meetings), SEDRIC has created a pool of international members to raise awareness on current gaps and promote sustainable solutions in surveillance and epidemiology.
Through these activities we convene experts in AMR surveillance and epidemiology to share knowledge. We listen to our member experts in order to move forward with our analysis and identification of gaps and solutions. We learn from one another so we can ensure we are best placed to offer expert recommendations.
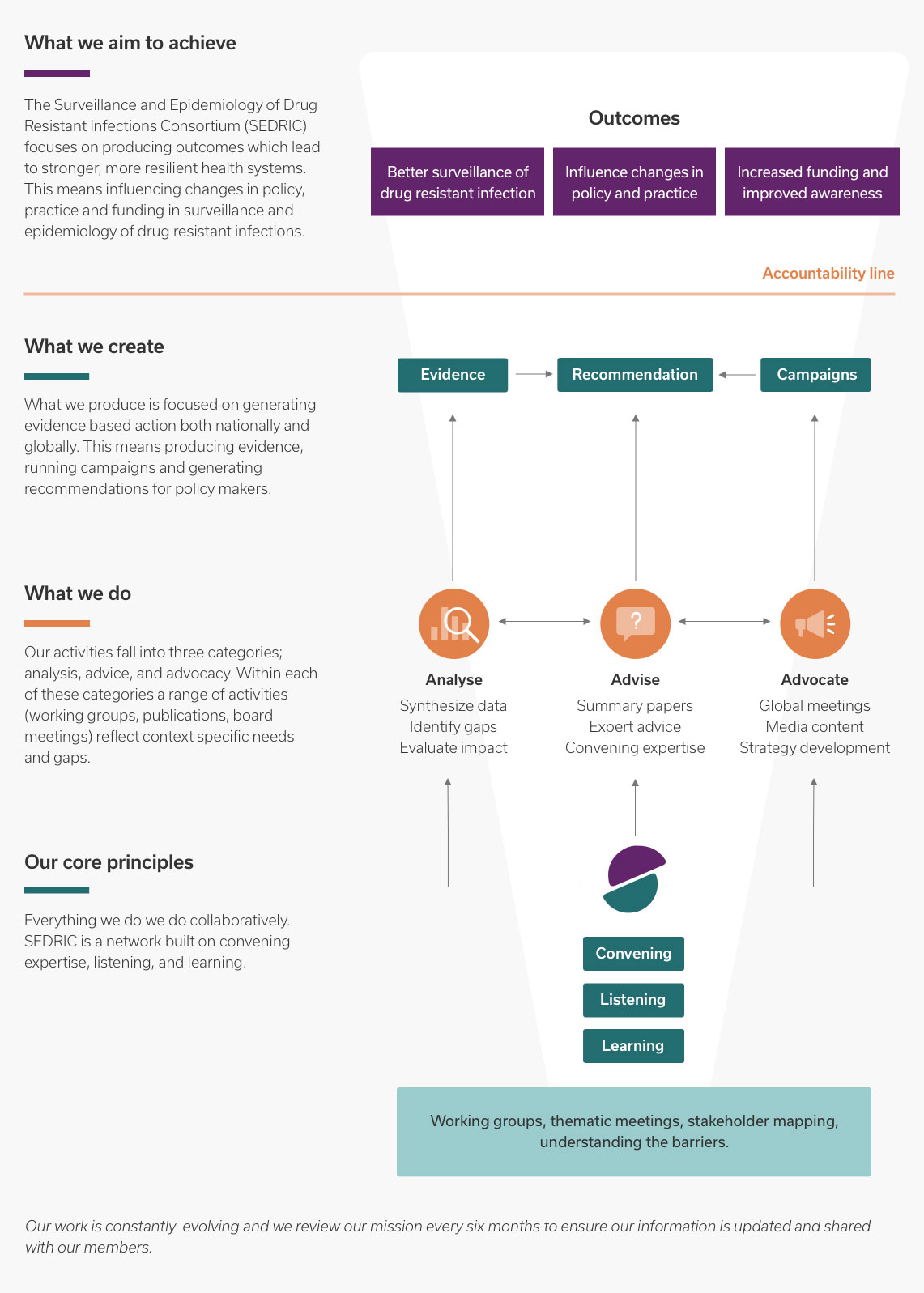
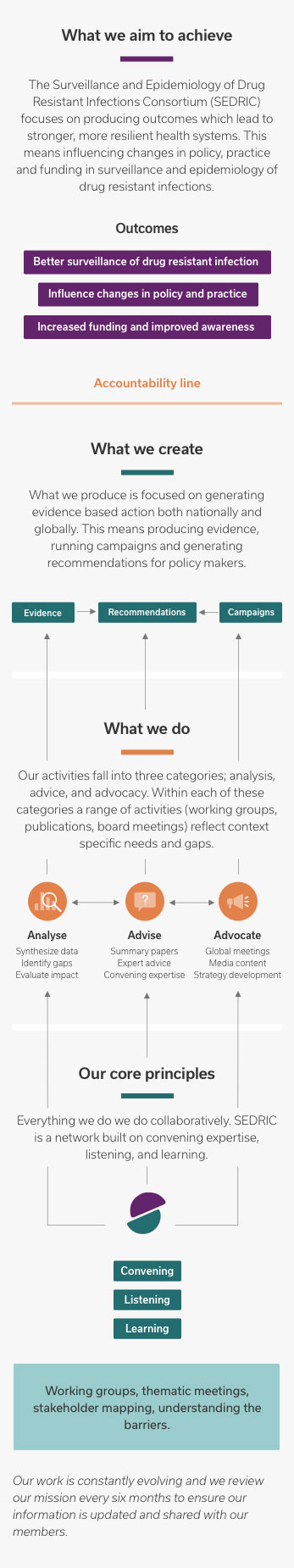
What we aim to achieve
The Surveillance and Epidemiology of Drug Resistant Infections Consortium (SEDRIC) focuses on producing outcomes which lead to stronger, more resilient health systems. This means influencing changes in policy, practice and funding in surveillance and epidemiology of drug resistant infections.
What we create
What we produce is focused on generating evidence based action both nationally and globally. This means producing evidence, running campaigns and generating recommendations for policy makers.
What we do
Our activities fall into three categories; analysis, advice, and advocacy. Within each of these categories a range of activities (working groups, publications, board meetings) reflect context specific needs and gaps.
Our core principles
Everything we do we do collaboratively. SEDRIC is a network built on convening expertise, listening, and learning.
How we are funded
SEDRIC is currently funded by Wellcome and receives support from the Drug Resistant-infections Priority Area team at Wellcome. Wellcome does not participate in the day-to-day governance of SEDRIC, but it is involved in appointing of SEDRIC board members.
Please note, SEDRIC is not a funding body and does not provide funding to other organisations or individuals.
Endorsements
“We know that good data will be essential if we are to successfully tackle drug-resistant infections, but what is also essential is that these data are available to those who need it. At SEDRIC we want to identify where gaps in data exist, what the barriers are preventing its full use and advocate for how these can be overcome at a national and international level. We coordinate expertise on surveillance and epidemiology from around the globe to advocate for better practices in all settings. We rely on the expertise of clinicians, microbiologists, vets and many others from all over the world to take an active role in contributing to our work and that is why our membership is so important.”
Sharon Peacock, SEDRIC Chair.
“Wellcome is proud to support the important work being done by SEDRIC. Progress to effectively control drug-resistant infections will reuire evidence-informed decisions. Having good, openly accessible data is central to Wellcome’s strategy to tackle antimicrobial resistance (AMR) globally. We must be able to inform data collection systems on where gaps exist and how to overcome existing barriers to collection so that data is available to inform treatment of patients and the public health response to AMR. This is why SEDRIC’s work will be invaluable in the global effort to stop superbugs.”
Tim Jinks, Head of Drug-Resistant Infections, Wellcome.
“Global action on antimicrobial resistance must be informed by good quality data that is available at the global, national and local level. SEDRIC identifies barriers to evidence-based decision making and advocates for more effective surveillance and epidemiology of drug-resistant infections. I fully support this important work, which is crucial if we are to stop superbugs.”
Sally Davies, UN Special Envoy on AMR, former Chief Medical Officer for England and Wales
How we are governed
SEDRIC has two governing entities:
The Board
Comprised of a chairperson and antimicrobial resistance (AMR) surveillance and epidemiology experts, the Board sets SEDRICs agenda and objectives, produces publications and holds votes on SEDRIC matters.
The Secretariat
The Secretariat is responsible for organising board meetings, implementing the board’s recommendations, supporting working groups, managing SEDRIC membership and running SEDRIC’s day-to-day operations.
Board members
The SEDRIC board has 11 members, with expertise spanning genetics, epidemiology, microbiology, public health and animal health. The current chair is Professor Nick Feasey.
The board will commission reviews and convene fixed-term working groups to address key issues in the fight against drug-resistant infection. This could include how to develop guidelines and tools to encourage data sharing, or how to translate scientific evidence into policy.

Nick Feasey is a clinician academic and Professor of Microbiology at the Liverpool School of Tropical Medicine. He is a consultant in medical microbiology and clinical infectious disease and he is based at the Wellcome Major Overseas Programme in Blantyre, Malawi, the “Malawi Liverpool Wellcome Trust Clinical Research Programme” (MLW)
His research is focused on the surveillance and management of bacterial bloodstream infection, and taking a one health approach to exploring the transmission of enteric pathogens and associated antimicrobial resistance determinant using genomics, spatial statistics and transmission modelling in collaboration with the Wellcome Trust Sanger Institute and CHICAS at the University of Lancaster.

Raheelah Ahmad (Deputy Chair)
Director for Global Engagement at the School of Health Sciences, City, University of London.
Read moreRaheelah is the Knowledge Mobilisation Lead at the NIHR Health Protection Research Unit (HPRU) for Healthcare Associated infections and Antimicrobial Resistance, and the NIHR HPRU Respiratory Infections, Imperial College London. She is a co-investigator at the NIHR HPRU Modelling and Health Economics and on the ESRC/UKRI project to address AMR in low resource settings (ASPIRES). This builds on her NIHR Fellowship in Knowledge Mobilisation (2016-2019) where she led research to evaluate sustained impact of interventions across the healthcare economy to address antimicrobial resistance.
Her previous research experience includes mixed method approaches to the study of innovation adoption at the organisational level and evaluation of public health interventions in a number of international contexts (Family medicine model in Bosnia & Turkey; Global fund interventions to address HIV and TB in Ukraine & Moldova; Maternal health interventions in Pakistan; national mental health policy in West Africa).
Following 10 years of management experience in the National Health Service England, Raheelah completed her doctorate in Health Management at Imperial’s Business School. She also has a Masters in Health Services Management from the London School of Hygiene and Tropical Medicine and a Mathematics degree from University College London. Raheelah is an associate member of the Health Group of the Management Department at Imperial’s Business School, member of the International Society for Global Health, Fellow of the Higher Education Academy (UK), Fellow of The Royal Society for Public Health and previously Senior Associate Editor of the peer reviewed international journal, Public Health.

Sharon Peacock
Professor of Public Health and Microbiology at the University of Cambridge, and Director of the COVID-19 Genomics UK (COG-UK) Consortium.
Read moreSharon is an academic clinical microbiologist at the University of Cambridge and the Wellcome Sanger Institute. She became the Executive Director and Chair of the COVID-19 Genomics UK (COG-UK) consortium (https://www.cogconsortium.uk) in April 2020. This was created to deliver large-scale and rapid whole-genome virus sequencing to local NHS centres and the UK government. COG-UK is made up of an innovative partnership of NHS organisations, the four Public Health Agencies of the UK, the Wellcome Sanger Institute and over twelve academic partners providing sequencing and analysis capacity. The virus genome data is combined with clinical and epidemiological datasets in order to help to guide UK public health interventions and policies.
In the decade prior to this, Sharon undertook research into the clinical and public health applications of pathogen sequencing, focusing on hospital-associated, antibiotic-resistant pathogens including MRSA (methicillin-resistant Staphylococcus aureus) and vancomycin-resistant Enterococcus faecium. Her group also use big data to explore biological processes relating to host-pathogen interactions.
Sharon is a non-executive director at Cambridge University Hospitals NHS Foundation Trust. She is a Fellow of the Academy of Medical Sciences, a Fellow of the American Academy of Microbiology, and an elected Member of EMBO. She was awarded a CBE for services to medical microbiology in 2015 and won the Unilever Colworth Prize for outstanding contribution to translational microbiology in 2018.

Rogier is a clinical microbiologist from the Netherlands who has worked in Vietnam since 2007. Rogier first headed the emerging infections group at the Oxford University Clinical Research Unit in Ho Chi Minh City. In 2015 he became director of the OUCRU unit in Hanoi.
In Hanoi, Rogier leads a community cohort for the study of human influenza. The OUCRU unit hosts a multidisciplinary research programme on antimicrobial resistance, including a Fleming Fund pilot investment. The programme includes laboratory diagnostics, new resistance mechanism discovery, clinical intervention trials and policy influencing with the responsible ministries.

Direk Limmathurotsakul
Head of Microbiology at Mahidol Oxford Tropical Medicine Research Unit
Read moreDirek has been the Head of Microbiology at MORU, a research collaboration between Mahidol University, the University of Oxford and Wellcome, since January 2012. He holds a Wellcome Intermediate Fellowship in Public Health and Tropical Medicine. He also runs his own fellowship-funded research programme on reducing the global burden of melioidosis.
Direk’s main research areas are melioidosis and antimicrobial resistance. He is also interested in public engagement and influencing policy change at a local and global level. He sits on the Thailand National Action Plan on Antimicrobial Resistance working committee.
By integrating routinely collected data from a range of databases, Direk has estimated that around an extra 19,000 deaths are caused by multi-drug resistant bacteria in Thailand each year. He has also estimated the antibiotic footprint of chicken meat in Thailand and proposed that labels on retail packs of meat should include data on antibiotic use.

Dr. Dawn Sievert leads the strategic direction, coordination, and investments of CDC’s cross-cutting scientific antibiotic resistance (AR) activities. Her work supports national goals outlined in the U.S. National Action Plan for Combating Antibiotic-Resistant Bacteria and ensures that AR projects and collaborations across the agency are appropriate and consistent with CDC scientific vision and priorities. As part of this role, Dr. Sievert provides the scientific leadership for CDC’s Antibiotic Resistance Laboratory Network and the CDC and FDA Antibiotic Resistance Isolate Bank. She is also Lead of the CDC Collaborating Center within the World Health Organization’s Antimicrobial Resistance Network.
Dr. Sievert previously served as the Associate Director for AR in CDC’s Division of Foodborne, Waterborne, and Environmental Diseases and as the Deputy Chief of Surveillance Branch in CDC’s Division of Healthcare Quality Promotion, where she provided scientific leadership for CDC’s National Healthcare Safety Network.
Prior to CDC, Dr. Sievert held roles as the chief scientist within a consulting company focused on new models of electronic automation and health information exchange in medicine and public health; quality improvement and infection control coordinator within a major healthcare system; AR program lead at Michigan’s state health department; and laboratory scientist focused on Alzheimer’s disease and multiple sclerosis research. Dr. Sievert received her PhD in Infectious Disease Epidemiology and BS in Microbiology from the University of Michigan in Ann Arbor, and MS in Epidemiology from the University of Illinois at Chicago.

Stuart is Principal of the Royal Veterinary College (RVC) at the University of London. An alumnus of the University of Glasgow, he became one of its youngest professors in 1996 and dean in 2005, before moving to the RVC in 2011.
Stuart is recognised as a specialist in veterinary epidemiology by the Royal College of Veterinary Surgeons (RCVS) and in veterinary public health by the European Board of Veterinary Specialists. He is a Fellow of the Royal Society of Biology and the Royal Society of Edinburgh. His research interests include zoonotic disease and antimicrobial resistance.
Stuart was President of the RCVS in 2014-15, a year which saw the launch of a new Royal Charter, the introduction of the courtesy title of ‘Dr’ for UK veterinarians, and an overhaul of the organisation’s 50-year old governance structures. Two major initiatives – Vet Futures and Mind Matters – were also launched. In 2015, Stuart ran the London marathon, raising £14k and awareness for mental health issues in the profession.
In his public service, he has been a trustee of The Donkey Sanctuary since 1996, and Chairman of trustees since 2007. He is a trustee of the University of London and sits on the board of the Food Standards Agency in the UK.

Jyoti Joshi
Antimicrobial Resistance (AMR) advisor at international centre for antimicrobial resistance solutions
Read more
Dr Jyoti Joshi MD is the Antimicrobial Resistance (AMR) advisor at the international centre for antimicrobial resistance solutions. She is a medical doctor specialized in Community Medicine and is an Adjunct Professor at Amity Institute of Public Health, Amity University, Noida, India.
Jyoti co-authored the Scoping Report on the antimicrobial resistance research landscape in India and as the Asia lead for the Global Antibiotic Research Partnership (GARP) project, she supports LMIC countries in Asia to develop and implement national action plans and develop policies to combat antimicrobial resistance. She has supported AMR Situation Analyses in Pakistan, Laos, and Bangladesh and advised the World Health Organisation for country case studies to explore ways to integrate AMR action plans into existing health programs. This contributed to the development of the WHO working paper ” Turning plans into action for antimicrobial resistance”: Jyoti is undertaking large multi-disciplinary research projects in India: first to explore potential for smart regulations for antibiotic use in India using a one health approach and another, to map the drivers of antimicrobial resistance in poultry in India.
Prior to CDDEP, Jyoti has worked with the Immunization Technical Support Unit, Ministry of Health and Family Welfare and the Ministry of Health, United Arab Emirates. Jyoti played a key role in strengthening the Adverse Events Following Immunization (AEFI) Surveillance system and establish the Secretariat for the National Technical Advisory Group on Immunization(NTAGI) in India. Her work contributed to strengthening immunization policy and several new vaccine introductions in India and UAE.

Mirfin Mpundu is the Head of Antibiotic Resistance (ReAct) Africa a Civil Society Organization (CSO) organization that articulates the complex nature of antibiotic resistance and its drivers. ReAct plays as a catalyst, advocating for and stimulating country, regional and global engagement on antibiotics resistance by collaborating with broad range of organizations, individuals and stakeholders. Mirfin has been involved in the development of AMR National Action Plans in several African countries. He is a member of several boards and technical working groups including the World Health Organizations Strategic Advisory Group (STAG) on antimicrobial Resistance.
Mirfin is also the Executive Director of the Ecumenical Pharmaceutical Network (EPN) a not for profit, independent organization committed to the provision of quality pharmaceutical services as a means to achieving global goals. A Registered Clinical pharmacist and Public Health Specialist with 20+ years of proven experience in public health, pharmaceutical supply chain management, clinical management, logistics and regulatory pharmacy practice experience. His experience also includes spearheading successful pooled procurement of pharmaceuticals & medical commodities at country and regional level, contract management, co-technical regional and global experience, quality assurance, organization strategy evaluation and development . He has an adept knowledge in resource mobilization, working with partners, data analysis, drug utilization review, operational research and capacity building.
Mirfin is also passionate about equitable access to quality-assured medicines and the inclusion and participation of Church Health Facilities within the global health agenda serving in hard to rich areas.

Souha Kanj is currently a tenured Professor of Medicine at the American University of Beirut Medical Center, Beirut, Lebanon, and Consulting Professor at the Duke University Medical Center, Durham, North Carolina, USA, where she also undertook her training in Internal Medicine and Infectious Diseases.
Professor Kanj is extensively published, with more than 220 papers in national and international journals such as Mycoses, Infection, Lancet Infectious Diseases and the Journal of the American Medical Association (JAMA).She has also been an invited author of numerous book chapters, journal reviews and UpToDate® cards and is currently Principal Investigator on research projects on topics related to antimicrobial resistance. Professor Kanj has contributed greatly to the work of the World Health Organization (WHO) in various programmes, such as the R&D Blueprint Annual Review of Priority Diseases, the Global Infection Prevention and Control Network, and the WHO Priority Pathogens List Project for Antimicrobial Resistant Bacteria. In 2020 she was appointed to serve on the WHO COVID-19 Guidance Development Group of experts (COVID-19 IPC GDG).
Professor Kanj is a fellow of the American College of Physicians (FACP), the Infectious Diseases Society of America (FIDSA), the Royal College of Physicians (FRCP), the European Society of Clinical Microbiology and Infectious Diseases (FESCMID) and the European Confederation of Medical Mycology (FECMM). She is a member of the scientific affairs committee of ESCMID and was elected to the executive committee of the International Society of Antimicrobial Chemotherapy (ISAC) in November 2019.
She has served on panels for international guidelines such as IDSA vertebral osteomyelitis and the recent ECMM global mucormycosis, and the rare yeasts guidelines.
In 2014, she was invited as a Visiting Scholar Professor at the Division of Infectious Diseases at Duke University Medical Center, and at Radboud University Medical Centre (UMC), Nijmegen, The Netherlands, in 2018.
Professor Kanj has been the recipient of numerous honours and awards throughout her career, including the Lebanese National Council for Scientific Research award in 2014 and the Abdul Hameed Shoman Award for researchers in the Arab world in 2017. In 2018, she received from Radboud University Medical Center, in Nijmegen the Valkhof professorship followed by an honorary degree in October 2020.

Dr Kamini Walia is a microbiologist by training and has subsequently trained in public health from Johns Hopkins. She is working as a Senior Scientist in the Division of Epidemiology and Communicable Diseases Division of Indian Council of Medical Research. She spent 2 years in PATH, as Director, Research and Development. During her 20 years of experience in the public health space, she has initiated and successfully steered numerous projects and programs of public health importance in the field of infectious diseases, reproductive and child health and non-communicable diseases. Dr Walia’s experience spans working on infectious diseases, including HIV/AIDS programs and heath technologies including vaccines and diagnostics. Dr Walia is currently leading the Antimicrobial Resistance Initiative of ICMR. She curated the National Essential Diagnostics for the country to improve the availability of diagnostics at all levels of health care. She is a former member of the WHO Scientific Advisory Group of Experts on Essential Diagnostics.
She is a member of:
· WHO Scientific Advisory Group of Experts on AMR Diagnostics
· Scientific Advisory Committee of GARDP
· Commissioner on Lancet Commission on Diagnostics
She is a recipient of ICMR’s Shakuntala Amir Chand Award, Indian National Science Academy, Young Scientist Award and NIH’s Fogarty Fellowship. She has received numerous fellowships and training from WHO, NIH, USA, IVI, Seoul, Pasteur Institute, France.
She has more than sixty publications in peer-reviewed journals.

Dr Atun is a Professor of Global Health Systems at Harvard University. In 2008-12 he was a member of the Executive Management Team of the Global Fund as Director of Strategy, Performance and Evaluation where he chaired the panel that oversaw annual investments of ~US$4 billion each year.
In 2006-2013 Dr Atun was a Professor of International Health Management at Imperial College London and Head of the Health Management Group. He is a visiting professor at the University of Kyoto, Japan and Imperial College London. He is a co-Investigator at the NIHR Health Protection Research Unit for Healthcare-Associated infections and Antimicrobial Resistance, Imperial College London.
Professor Atun’s research focuses on health system transformation and innovation. He has published more than 400 articles in leading journals including NEJM, Lancet, JAMA, Academy of Management Journal, Lancet Oncology, Lancet Global Health. He has led and participated in More than 10 Lancet Commissions. In 2020 he was recognised by Web of Science, Clarivate as one of the World’s Highly Cited Researchers.
Dr Atun has advised many governments, the World Bank, WHO and leading corporations. He served as a member of the U.S. National Academy of Medicine Committee on Health Systems and on the Advisory Boards of WHO Research Centre for Health Development in Japan and the Norwegian Research Council’s Programme for Global Health Research. He Chaired the STOP TB Partnership Coordinating Board in 2009-2011 and was a member of the UK Medical Research Council’s Global Health Group. In 2013-19 he was a member of the Advisory Committee to the Editors, Disease Control Priorities 3. In 2019-20 he was a senior advisor to the G20 Presidency. He is a member of the Longitude Prize Committee – the largest science prize in the world.
Previous board members
Alison Holmes
Professor of Infectious Diseases, Imperial College London
Iruka N Okeke
Professor of Pharmaceutical Microbiology at University of Ibadan, Nigeria
Keiji Fukuda
Clinical Professor and Director, School of Public Health, University of Hong Kong
Nandini Shetty
Clinical Microbiologist at University College London Hospitals and Public Health England
Gemma Buckland Merrett
Science Lead Drug Resistant Infections at Wellcome Trust
SEDRIC secretariat team

Jamie is part of the Drug Resistant Infections team at Wellcome Trust. He previously worked at Oxford Policy Management in the Project Support Unit and as a Project Evaluator in East Africa, conducting monitoring and evaluation work for GlobalGiving UK. Jamie recently completed his master’s in Health Policy, Planning and Financing, awarded jointly by the London School of Economics and Political Science and the London School of Hygiene and Tropical Medicine.
Become a member
Are you working in AMR surveillance and epidemiology? Join SEDRIC today to start communicating and collaborating with our community of experts.